 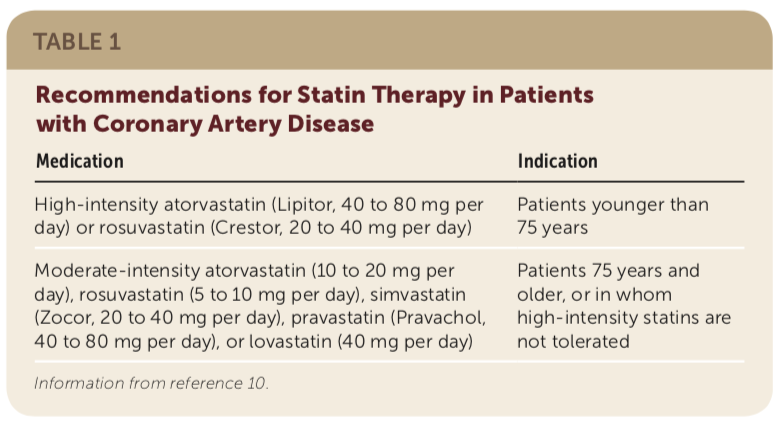
Sodium-glucose cotransporter 2 (SGLT-2) inhibitors act in the proximal tubule to increase urinary excretion of glucose and sodium, leading to a reduction in HbA1c, weight, and BP and in randomized clinical trials, significant reduction in ASCVD events and heart failure. Two classes of glucose-lowering medications have recently demonstrated a reduction in ASCVD events in adults with T2DM and ASCVD. Several classes of medications have been shown to effectively lower blood glucose but may not affect ASCVD risk including the often-used sulfonylureas. Compared to lifestyle modifications, metformin resulted in a 32% reduction in micro- and macrovascular diabetes-related outcomes, a 39% reduction in myocardial infarction, and a 36% reduction in all-cause mortality. For younger individuals, or those with a mildly elevated HbA1c at the time of diagnosis of T2DM, clinicians can consider a trial of lifestyle therapies for 3-6 months before drug therapy.įirst-line therapy to improve glycemic control and reduce CVD risk is metformin. Other risk factors should be identified and treated aggressively. At least 150 minutes/week of moderate to vigorous physical activity (aerobic and resistance) in T2DM lowers HbA1c about 0.7% with an additional similar decrease by weight loss. 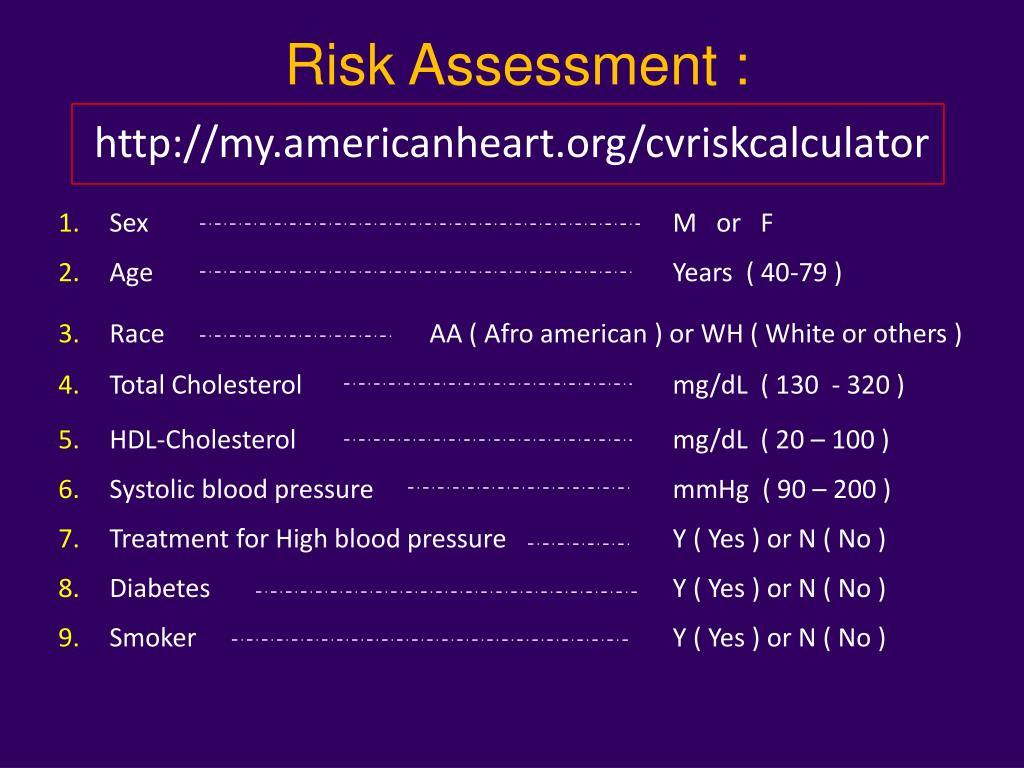
Among options include the Mediterranean, DASH, and vegetarian/vegan diets that achieve weight loss and improve glycemic control. All with T2DM should undergo dietary counseling for a heart-healthy diet that in T2DM lowers CVD events and CVD mortality. The development and progression are heavily influenced by dietary pattern, physical activity, and body weight. Adults should be categorized into low (130 mg/dl, and ankle-brachial index (ABI) 6.5%, is a metabolic disorder characterized by insulin resistance leading to hyperglycemia. The guideline suggests the race- and sex-specific Pooled Cohort Equation (PCE) ( ASCVD Risk Estimator Plus) to estimate 10-year ASCVD risk for asymptomatic adults aged 40-79 years. Electronic and paper chart risk estimators are available that utilize population-based and clinical trial outcomes with the goal of matching need and intensity of preventive therapies to absolute risk (generally 10 years) for ASCVD events.For those aged 20-59 years not at high short-term risk, the 30-year and lifetime risk would be reasons for a communication strategy for reinforcing adherence to lifestyle recommendations and for some drug therapy (e.g., familial hypercholesterolemia, hypertension, prediabetes, family history of premature ASCVD with dyslipidemia or elevated lipoprotein Lp). 
For adults aged 20-39 years and those aged 40-59 years who are not already at elevated (≥7.5%) 10-year risk, estimating a lifetime or 30-year risk for ASCVD may be considered ( ASCVD Risk Estimator Plus). For those aged 20-39 years, it is reasonable to measure traditional risk factors every 4-6 years to identify major factors (e.g., tobacco, dyslipidemia, family history of premature ASCVD, chronic inflammatory diseases, hypertension, or type 2 diabetes mellitus ) that provide rationale for optimizing lifestyle and tracking risk factor progression and need for treatment. Assessment of ASCVD risk is the foundation of primary prevention.The guideline emphasizes patient-physician shared decisions with a multidisciplinary team-based approach to the implementation of recommended preventive strategies with sensitivities to the social determinants of health that may include specific barriers to care, limited health literacy, financial distress, cultural influences, education level, and other socioeconomic risk factors related to short- and long-term health goals. The focus is primary prevention in adults to reduce the risk of ASCVD (acute coronary syndromes, myocardial infarction, stable or unstable angina, arterial revascularization, stroke/transient ischemic attack, peripheral arterial disease), as well as heart failure and atrial fibrillation. The guideline is a compilation of the most important studies and guidelines for atherosclerotic CVD (ASCVD) outcomes related to nine topic areas.The following are key perspectives from the 2019 American College of Cardiology/American Heart Association (ACC/AHA) Guideline on the Primary Prevention of Cardiovascular Disease (CVD): 
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
